Dr Evelyn Wesangula
East Central and Southern Africa Health Community (ECSA-HC)

Dr Jackline Kiarie
Institute of Capacity Development, Amref Health Africa
Antimicrobial resistance (AMR) demands a coordinated African continental response. It’s time to accelerate national plans and regional action in Africa.
Africa has the highest AMR mortality rates globally.1 One in five bacterial infections in Africa is now resistant.2 By 2050, Africa is projected to bear 40% of global AMR-related deaths.3 Without intervention, 4 million people in Africa will lose their lives every year from AMR-related illnesses.
We must turn the tide on AMR
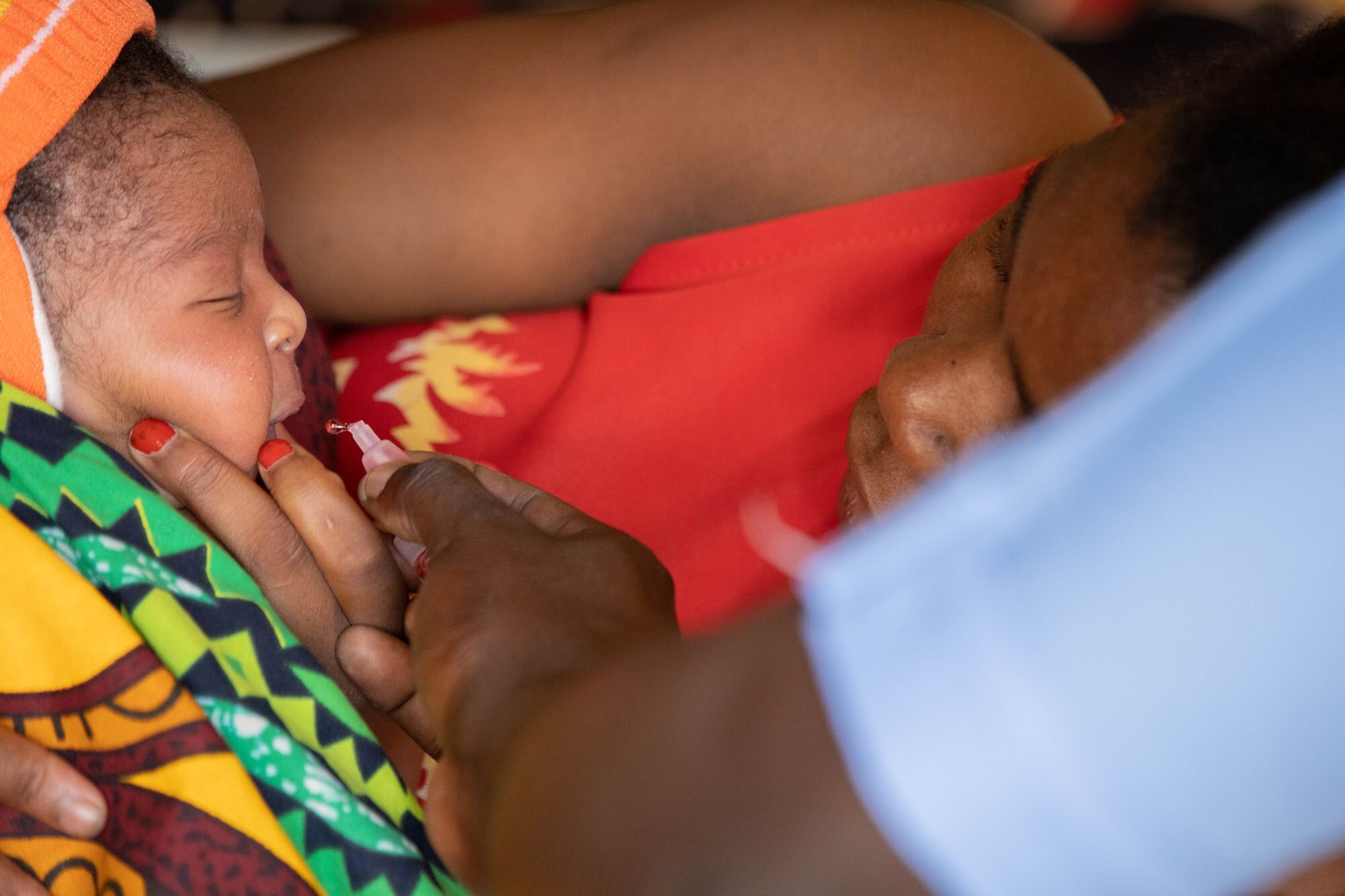
When vaccines and diagnostics are out of people’s reach, illnesses are treated blindly with broad-spectrum antibiotics and preventable infections spread unchecked. An Africa CDC and African Society for Laboratory Medicine study across 14 countries found that only 1.3% have sufficient bacteriology capacity. 4 Twenty-six percent of pharmacy healthcare workers surveyed in 28 African countries thought that antibiotics can be used to treat viral infections,5 and 55% of people in Africa self-prescribe antibiotics.6
These patterns of misuse also affect animal health. Amref Health Africa found that one in five animal owners in Burkina Faso, Cameroon, Ethiopia, Kenya, and Zambia occasionally use human medicine to treat animals due to gaps in veterinary care. 7
Yet, across many African nations, there is limited access to quality antibiotics. Over-the-counter sales of substandard or counterfeit drugs fuel antibiotic misuse and resistance.
These inequities create the perfect conditions for resistant strains to emerge and spread.
Strong continental frameworks to stop the spread
The African Union Taskforce on AMR provides a continental coordination mechanism, driving One Health policy priorities and adoption of AMR National Action Plans. It plays an essential role in feeding Africa-specific evidence and integrating African priorities into global action platforms like the Quadripartite Joint Secretariat on AMR.
These cooperative partnerships work to unite human, animal, plant and environmental health actors. By coordinating surveillance and evidence generation projects like Mapping Antimicrobial Resistance and Antimicrobial Use Partnership (MAAP), they can produce data to guide national policy. They are coordinating training and lab strengthening to make AMR testing more available and reliable. With increased laboratory capacity to collect and analyse samples from hospitals, clinics, farms and the environment, we can better detect resistant strains .
Coordination challenges slow down the response
These are strong continental One Health frameworks, but implementation often remains siloed. National human health, animal health, and environment ministries run separate surveillance data systems and regulatory policies.
Lack of systems to generate reliable data, inconsistent data sharing and lack of harmonised standards delay timely detection and response. Without national data feeding regional platforms, it is difficult to coordinate regional data analysis to map patterns and trends. This uneven capacity creates ‘blind spots’ where resistant strains can spread across borders with no early warning.
Limited domestic financing and heavy donor dependence undermine sustainability. Nearly a decade on from the development of National Action Plans, just 5% of African NAPs are fully funded. And without mandatory reporting, few countries enforce stewardship or report progress. Private sector and community actors are often underrepresented in AMR coordination forums. Behaviour change communication campaigns are often sporadic and not coordinated across Africa.
Our joint continental action and partner driven efforts
create a regional architecture to strengthen systems.
African leadership is driving AMR Action
Initiatives like the African Leadership for AMR Action, led by Amref Health Africa and funded by GSK, are helping to bridge the gap.
It brings together private and community health sectors, One Health leaders in national governments and regional coordination bodies to strengthen leadership and local ownership for AMR action. It supports cross-sector workforce capacity building on AMR to drive more effective Antimicrobial Stewardship. It drives better community AMR understanding through integrating AMR education and awareness interventions into community health programmes and coordinating advocacy and media campaigns. Working at the national and regional levels, it enhances multisectoral action to drive cohesive and sustainable AMR mitigation efforts.
Similarly, the Health Emergency Preparedness Response and Resilience project, spearheaded by the East Central and Southern Africa (ECSA) Health Community and funded by the World Bank, has prioritised building regional and country level capacities to better implement AMR interventions.8 It aligns countries to common standards and its Ministers’ Conference and Community of Practice on AMR and Infection Prevention and Control convenes stakeholders, optimises regional expertise, and keeps AMR high on the political agenda.
Our joint continental action and partner driven efforts create a regional architecture to strengthen systems. With evidence-based interventions, stronger coordination, sustainable financing and cross-sector enforcement, we are driving progress in the fight against AMR. In this way, together, we will safeguard Africa’s future health.
[1]World Health Organization Africa. 2024. Addressing the challenges of antimicrobial resistance in Africa.
[2]World Health Organization. 2025. Global antibiotic resistance surveillance report 2025.
[3]Institute for Health Metrics and Evaluation. 2024. The Lancet. Table S17, Appendix 1.
[4]Osena, Gilbert et al. Antimicrobial resistance in Africa: A retrospective analysis of data from 14 countries, 2016-2019. PLoS medicine vol. 22,6 e1004638. 24 Jun. 2025, doi:10.1371/journal.pmed.1004638
[5]Agiri O, Osena G, Bahati F, Dill D, Kalanxhi E, Ashiru-Oredope D, et al. Knowledge, attitudes and practices survey on antimicrobial resistance and stewardship among pharmacy healthcare workers in 28 African countries. BMJ Global Health. 2025;10:e019151. https://doi.org/10.1136/bmjgh-2025-019151
[6]Yeika, Eugene Vernyuy, et al. 2021. Comparative assessment of the prevalence, practices and factors associated with self-medication with antibiotics in Africa. Tropical medicine & international health: TM & IH vol. 26,8 (2021): 862-881. doi:10.1111/tmi.13600
[7]Amref Health Africa. Antimicrobial Landscape Analysis in Select African Countries Report (Burkina Faso, Cameroon, Ethiopia, Kenya, Zambia).
[8]Wesangula, E.; Chizimu, J.Y.; Mapunjo, S.; Mudenda, S.; Seni, J.; Mitambo, C.; Yamba, K.; Gashegu, M.; Nhantumbo, A.; Francis, E.; et al. A Regional Approach to Strengthening the Implementation of Sustainable Antimicrobial Stewardship Programs in Five Countries in East, Central, and Southern Africa. Antibiotics 2025, 14, 266.