Prof. Jesús Rodríguez-Baño
President-Elect of European Society of Clinical Microbiology and Infectious Diseases (ESCMID)
It will take a well-planned global effort if we are to prevail in our fight against antibiotic-resistant microorganisms.
For the world as a whole, a growing number of microbes causing pneumonia, urinary or intra-abdominal infections, to name just a few – are becoming harder to treat as the drugs to treat them become less effective. This problem also includes tuberculosis, malaria or HIV. For example, in 2016, 490,000 people developed multi-drug resistant tuberculosis globally, including in the UK, and drug resistance is starting to complicate the fight against HIV and malaria, as well. Also, the proportion of gram negative bacteria showing resistance to carbapenems, the last resource for many infections, has dramatically increase in the last decade worldwide.
An infection epidemic
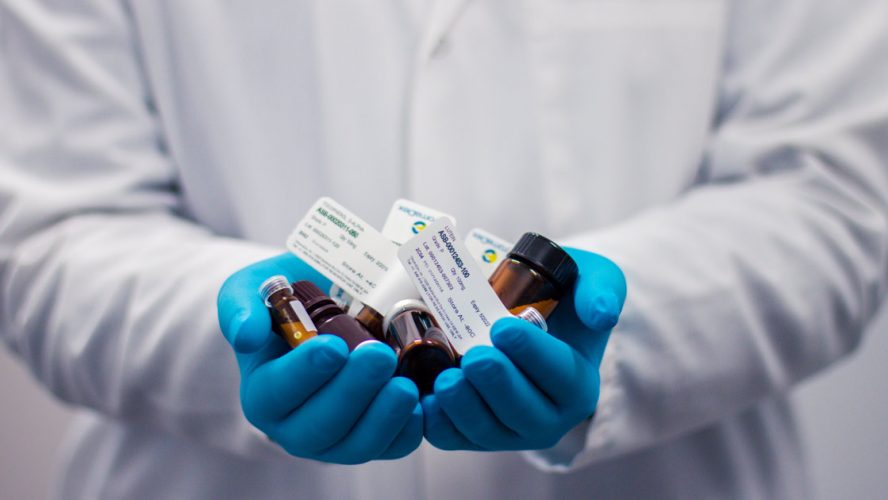
Antimicrobial resistance (AMR) happens when microorganisms (such as bacteria, fungi, viruses, and parasites) are not susceptible to the action of antimicrobial drugs (such as antibiotics, antifungals, antivirals, antimalarials, and anthelmintics). Resistant microorganisms are sometimes referred to as “superbugs” by the media. AMR occurs naturally over time. However, antibiotic resistance is accelerated by the misuse and overuse of antibiotics, as well as poor infection prevention and control. Resistant organisms can spread easily today between distant geographical areas as a result of globalisation.
Infections caused by antimicrobial-resistant organisms are usually associated with worse outcomes. Life without effective antibiotics can also mean that medical procedures such as cancer chemotherapy, organ transplantation and other types of surgery suddenly become very high risk in some patients.
Global effort needed to tackle antibiotic resistance
It is now accepted that there needs to be a global action plan on AMR. The most urgent need is on greater investment in research and development of new antimicrobial medicines or non-antibiotic approaches, vaccines, and diagnostic tools to help clinicians identify when antimicrobial drugs are required. But other actions are needed, including promotion of appropriate use of antimicrobials in human and non-human environments, implementing better systems for surveillance of antibiotic-resistant organisms, improvement of sanitary conditions in developing countries, and enhanced infection prevention and control activities.
In the development of new drugs to treat such organisms, the pharma industry, of course, has a leading role, but cost-effective product development is intrinsically difficult. To facilitate the implication of industry in this field, a different model of commercial return may be needed. Academia and politics have a role to play in this -– to explore what needs to change to ensure that industry finds it attractive to invest in discovering and developing new drugs or new treatment approaches, and to collaborate in the process. Additionally, publicly funded academic research in some existing but neglected old antimicrobial agents may also provide some partial solutions to the problem.
Solving the problem is clearly complex; single, isolated interventions will have limited or no impact at all. It will take sustained education of professionals and society, appropriate investments in critical areas and enhanced scientific research to make the progress we need to tackle antimicrobial resistance. To achieve this, AMR must be a priority for politics, scientific organisations, educators, researchers and healthcare professionals.